Hartford Reducing Barriers to COVID-19 Vaccine Access in Minority Communities
By Julia Gintof
Journalism 2001
May 2021
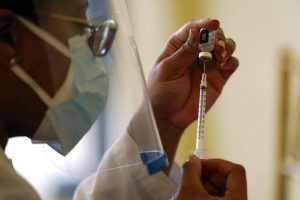
On April 6, mobile units pulled into the parking lot of the Swift Factory in Hartford with one mission: to deliver COVID-19 vaccines to the community.
Hundreds of residents lined the street for the no-appointment vaccination center awaiting a shot that may end up saving their lives.
“It’s important to have walk-up clinics so people can have access to it… for us to carve out spaces for those who actually live in the city,” Ayesha Clarke, deputy director at Health Equity Solutions, said.
The North End of Hartford, home to a minority-dense population, has seen a lower percentage of vaccinated individuals during the initial stage of rollout.
According to Connecticut Department of Health Statistics, first dose coverage across the state by February saw Black and Hispanic residents at a significant deficit, receiving half the vaccinations on average in comparison to their white counterparts.
This reflects CDC data across the country. Within the first two months of rollout, white individuals across the U.S were vaccinated at almost twice the rate of Black Americans and nearly two-and-a-half that of Hispanic Americans.
The disparity has raised wider concern surrounding equity within the American healthcare system, as organizations push local and state governments to address the issue.
“The biggest cause of this is the systemic racism in all of our policies and practices that go back historically,” Communications Director of Race Forward Cheryl Blakemore said. A national organization dedicated to working with local governments to provide equal opportunity for communities of color, Race Forward has been vocal in exposing vaccine inequity.
While the United States Black and Hispanic population has been adversely impacted by the virus, posting greater infection and death rates, the government’s initial methods of vaccine rollout seemed to disregard some of those who need it most.
“If you don’t have a computer, or access to internet, or a phone that you would have that type of capability, then you can’t sign up for the vaccine… you can’t get notifications like other people can,” Blakemore said.
The main underlying issue is access. Clarke emphasized that the inability to register for a vaccine due to factors such as time conflicts, limited daycare options, or lack of transportation is a real issue for many minority residents.
“I live in an inner-city and the individuals who are going to our local CVS and making appointments are not those who live in the city,” she said.

Clarke added that people outside of her community have greater advantages such as access to technology and knowledge of vaccination sites. This inhibits other minorities and residents of the city from being able to fill those slots.
In an effort to remove these barriers to access, Hartford Mayor Luke Bronin tweeted that the Connecticut Health Department is making walk-up clinics more of a priority, as Gov. Ned Lamont recently announced a partnership with Health Equity Solutions.
“They’re hearing it now,” Clarke said. “I understand that’s why they now have the funding that’s appropriate to help provide resources to ensure that we are reaching those minority populations.”
A local organization dedicated to achieving equality within the healthcare system, Health Equity Solutions has brought the need to vaccinate communities of color to the forefront of conversation.
“Having these mobile sites is bringing it to where they are and giving them opportunity,” Clarke said.
But delivering the vaccine to high-need areas is only one hurdle in reaching the individuals within them.
“There is a longstanding mistrust in communities of color,” Blakemore said.
The Tuskegee Experiment, an U.S study conducted in the 1930’s, is just one example of unethical public health experiments conducted on minority communities. Throughout a period of nearly 40 years, researchers used hundreds of African American men as guinea pigs as they observed the deadly progression of syphilis and neglected to offer aid.
It is historical examples such as this for the Black population as well as immigration concerns for those within the Hispanic community that have caused significant wariness of the American healthcare system.
Mistrust is widespread across the state of Connecticut, Clarke said, emphasizing the importance of working to dispel hesitations within these minority communities.
“You have to be able to get people to feel like they can trust the vaccine and understand the consequences of why they need to take it — to save their life, their families lives, lives of people in their community,” Blakemore added.
Statistician for the UConn Health Disparities Institute Emil Coman said mending the bridge between the minority community and the healthcare system needs to come from community-trusted sources.
“Minorities, having a higher level of distrust, should be reached more directly,” he said, citing pastors, ministers, and even barbers as possible change-makers.
Clarke said that much of the hesitancy within the minority community is not solely rooted in past experience, rather a lack of trust in unknown doctors who most commonly don’t look like them.
“I feel like we use the hesitancy as an excuse not to help support the minority community,” she said. “If you really talk to them they just want questions answered and they want to see a clinic in their own city.”
She outlined the strides that Health Equity Solutions has made toward promoting greater education and rebuilding trust among minority individuals across Connecticut.
“We have clinicians of color, whether they are medical doctors or APRNs, and have created a speakers bureau to help have their questions answered,” she said.
Blakemore emphasized the importance of education and outreach as well. She commended the Biden Administration, which recently released $250 million in grants to local governments across the country. These funds are being allocated to local organizations to aid in health education efforts.
As the COVID-19 vaccine is now actively being delivered to adversely affected communities, Blakemore and Clarke touched on the initial unequal distribution as a wider issue among the American healthcare system.
“It is based in systemic racism. How our society as a whole forgets about minority communities,” Clarke said. “There are always barriers to health, COVID just heightened it, and exacerbated it.”
The walk-up clinics in the North End of Hartford are just one step in tackling a much more pervasive issue, one that HES is working on diligently.
As of April 22, the percentage of Connecticut’s Black and Hispanic population that have received at least one dose of the COVID-19 vaccine is still lower in nearly every age bracket when compared with the white population, according to government data.
This outlines that there is still work to be done to ensure equitable distribution.
Blakemore hopes the COVID-19 pandemic can be yet another step towards change in terms of closing the healthcare gap.
Part of this effort, she said, is “bringing communities to the table with government to address what issues already exist,” a large part of what Race Forward has dedicated itself to.
“Where they think their policies are fine and equitable they absolutely aren’t and we need to help develop solutions,” she said.
Leave a Reply
You must be logged in to post a comment.